Symptoms, Causes and Practical Advice
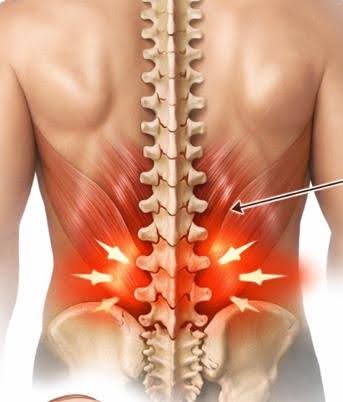
Mechanical or non-specific low back pain is by far the most common type of back pain I see
in clinic.
In nearly 20 years as a chiropractor at Active Health in Portsmouth, I would estimate that
this category alone accounts for well over half of all low back cases I treat and affects all
ages.
The reassuring news is that this type of back pain is rarely serious, often very treatable, and
usually responds well once the right aggravating factors are identified.
My aim on this page is to help you understand what’s really going on — and what you can
do about it.

What This Page Will Help You Understand
After reading this page, you should understand:
– What mechanical / non-specific low back pain actually means
– Common symptoms and patterns I see in clinic
– Why muscles and joints become painful
– What usually helps (and what often keeps it hanging around)
– What Products I Recommend to Aid Recovery
– Practical lifestyle and desk-based changes
– When to seek further medical advice
NB: If your pain travels down your leg, you may also want to read my Sciatica page (LINK).
If sitting or bending clearly worsens your pain, my Disc Bulge / Herniation page may be more
relevant (LINK).
What Is Mechanical (Non-Specific) Low Back Pain?
“Non-specific” sounds unhelpful…but it simply means that the pain is coming from muscles,
joints, ligaments or soft tissues, rather than a disc, nerve compression or serious condition.
You may often wonder what exactly is it that’s causing your back pain…and even more
confusing, why does the pain keep moving around!? The truth is that even after years of
dealing with these issues, it can be quite hard to tell as it might be one or a combination of
all the tissues mentioned above.
So basically, what medical people are really saying is:
We know the back is irritated
We know it’s not one of the more serious problems
We don’t want to admit that we don’t know EXACTLY which structure is causing the
problem!
Mechanical pain is influenced by movement, posture and load — hence the name. For
example, although I don’t generally get low back pain, I remember in the summer after I did
a lot of digging at my allotment, my low back was a bit stiff and achy.
Nothing damaged…just irritated. It got better quickly after a rest. However, if I then had to
dig every day through-out the summer, my back would be at risk of developing a mechanical
issue.

Common Symptoms I See in Clinic
Mechanical low back pain often presents with:
Ache or stiffness across the lower back
Pain on one or both sides
Tightness after sitting or standing too long
Pain that eases with gentle movement
Reduced flexibility
Morning stiffness that improves as you get moving
You might notice how it fluctuates…better one day, worse the next. I see this a lot.
CLINIC NOTE: Many patients tell me “It’s not agony, I’m just always aware of it but
occasionally it flares up.”
That’s a classic mechanical pattern.
Why Does Mechanical Back Pain Happen?
One thing I’ve learned over the years is that mechanical back pain is rarely caused by one
single event.
It’s usually the accumulation of small stresses over time.
Common contributors include:
Prolonged sitting (especially slumped)
Poor desk or work setup
Repetitive bending or twisting
Lack of movement variety
Reduced core or hip strength
Poor sleep and recovery
Stress (yes — it matters)
AND most commonly… a combination of all of the above.
This is why people often say:
“I didn’t do anything to cause it.” (You did, you just didn’t realise it)
In reality, the back has simply reached its tolerance threshold
Why It Often Doesn’t Just Go Away
One of the most common reasons mechanical back pain lingers is because people continue
doing the very things that caused it.
For example:
Sitting all day at work and then in a poor position on their sofa in the evening
Working at a poorly set-up desk
Exercising hard once a week, then not moving much in between
Exercising too hard several times/week
Your back doesn’t need perfection — it just needs better balance.
What Usually Helps Mechanical Back Pain?
- Improving Desk and Sitting Setup
This is one of the highest-impact changes I see in clinic.
Helpful steps include:
Improving chair support (see recommended chairs LINK)
Using a lumbar support cushion for office and car (LINK)
Raising screens to eye level
Standing up every 30–45 minutes
Using a sit-stand desk to change positions (LINK)
I cover this in detail on my Desk Setup Guide (LINK).
TOP TIP: It’s not just your work and driving position that needs attention. Take note also of
how you are sitting;
On the sofa
When socialising (at home or out)
- Regular, Gentle Movement
Spines like to move.
Helpful habits include:
Short walks spread through the day
Gentle low back mobility exercises (LINK)
Changing positions often
Avoiding “all-or-nothing” activity patterns
True Story: I had a patient in her 30’s once who had a low back problem that just kept on
recurring. Circumstances arose where she signed up for a charity walking event (if I
remember rightly, it was a 26 mile walk).
She knew she needed to put some training in to be able to complete the walk so started
walking most days over a couple of months—starting off gently and gradually increasing.
As a biproduct from this, she noticed over the coming months that her low back problem was
the best it had been for years!
I’ve added this story in just to show how a new regular positive habit can make such a big
difference!
- Building Load Tolerance (Long-Term Fix)
Once pain settles, the goal is to help your back tolerate everyday loads again.
This usually means:
Simple core and glute activation
Gradual strengthening
Practising good bending mechanics
Progressing slowly, not rushing
See my Beginner Low Back Exercises page (LINK) to get started.
True Story: My best friend is a gardener. He developed a mechanical low back problem over
the course of several months which started to affect his work as well as his home life (for
example he was struggling playing football with his sons)
On top of my treatment, he started regularly doing 10-15 minute morning yoga sessions
gradually progressing to strength work over the course of 2 months. This improved his spinal
mobility and stability.
It wasn’t immediate but gradually his back started to improve until he was pain free again! I
was really pleased with the result.
- Improving Sleep and Recovery
Poor sleep = poor healing.
Helpful changes may include:
A more supportive mattress or topper (LINK)
A small pillow between knees for side sleepers
A well supported pillow (Link)
Reducing evening screen time
Managing stress levels
Many of my patients just know when their mattress isn’t helping — trust your instinct.
How Long Does It Take To Improve?
This is one of the most common questions I’m asked and one of the hardest to answer
accurately.
As a general guide:
Mild flare-ups: 1–3 weeks
Moderate symptoms: 4–6 weeks
Persistent or recurring pain: several months
Recovery depends heavily on:
Daily habits
Activity balance
Sleep and stress
How consistently changes are applied
Top Tip: The more things you can improve on, the higher the likelihood of success!
The good news? Mechanical back pain responds very well when the environment is right.
When to Seek Further Medical Advice
You should seek urgent medical help if you experience:
Loss of bladder or bowel control
Numbness around the groin or genitals
Progressive leg weakness
Severe or rapidly worsening pain
These symptoms are not typical of mechanical back pain and should never be ignored.
Final Thoughts
Mechanical low back pain is extremely common and quite frankly an absolute nuisance! But
it doesn’t have to become permanent.
Most people improve when they:
Reduce aggravating habits
Improve desk and posture setup
Move more, but with better balance
Build strength gradually
Please use the links on my page to explore:
Desk setup advice
Posture guidance
Exercises
Practical tools that support recovery
Take it step by step — backs usually respond well when given the right conditions. Good
luck!
